The intestine - an organ with many superlatives
Our intestine is an organ with remarkable attributes. During a lifetime, it digests an estimated 50 tons of food and another 50.000 liters of liquids. Moreover, the gut is of fundamental importance for the immune system. Did you know that the largest part of our body’s immune cells is located in our bowel wall? The reason lies in the fact that the gut with its enormous surface area of about 300 square meters constitutes the largest interface of our body to the environment. Through this interface, the gut is constantly exposed to dietary constituents and potentially hazardous bacteria of the microbial flora. Speaking of the microbial flora: The human gut is home to an estimated 100 trillion bacteria, about 10 times as many cells as those who make up the human body.
The intestinal barrier is maintained by a single cell layer of epithelial cells. These cells have important functions in taking up nutrients from our food and in preventing the uncontrolled access of gut luminal content into our body. In a way, the intestinal epithelium can be regarded as a heavily guarded border.
Underneath the epithelium, deeper within the bowel wall, reside cells of the intestinal immune system. These cells can be regarded as the watch-dogs of the epithelial barrier. They have the fundamental task to control dietary constituents and bacteria crossing the epithelial barrier. Their delicate task is also to make the important decision of whether these constituents might be harmful (like pathogens) or harmless, whether they should be attacked or tolerated, respectively.
Experimental data from our group demonstrate that independent from each other, a defect in intestinal epithelial cell function as well as a dysregulated immune response of lymphocytes can lead to a breakdown of the immunological balance in the gut. As a consequence, inflammatory bowel disease (Crohn’s disease and ulcerative colitis) can develop. Another consequence of uncontrolled immune responses in the gut might be the manifestation of chronic inflammation in other parts of the body and the development of colorectal cancer.
1) Cell death regulation in intestinal epithelial cells and its role in health and disease
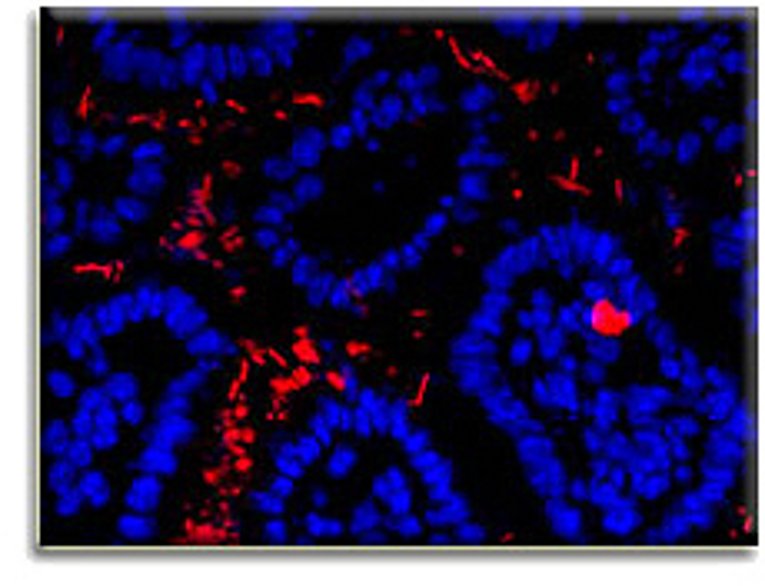
The human gut harbors an enormous number of bacteria (picture on the right, red staining). These bacteria are usually harmless and even help our body in absorbing nutrients. However, if they invade the bowel wall in an uncontrolled way (single red stained cell in the image to the right), these bacteria can become harmful and cause inflammation. To prevent the access of bacteria to the bowel wall, the gut is coated with a thin layer of epithelial cells (blue stained cells), which serves as a barrier. It is becoming more and more clear that intestinal epithelial cells are highly specialized cells with important functions for innate immune defense. In addition to establishing a tight physical barrier, they produce substances that can keep bacteria at a distance or even kill them. The cellular processes that maintain this barrier function and therefore a healthy gut are largely unknown. Investigation of the molecular mechanisms of the epithelial barrier is one of the topics of our group. Intestinal epithelial cells are also at the focus of our research on the development of colorectal cancer, since most tumors in the gut originate from these cells.
Cell survival and cell death within the intestinal epithelium have to be strictly regulated to prevent inflammation and cancer development in the gut. We have recently discovered necroptosis, a new kind of cell death, in intestinal epithelial cells. Dysregulation of necroptosis leads to the loss of Paneth cells, cells with important functions for the epithelial defense against bacteria. Ultimately, excessive necroptosis results in intestinal inflammation. Using molecular biological methods and experimental disease models of gut inflammation and cancer we investigate in detail the function and regulation of apoptosis, necrosis and necroptosis in the intestinal epithelium. We look at death receptor signaling induced by TNF-alpha and the roles of intracellular signaling networks regulated by CASPASEs, STATs (signal transducer and activator of transcription), SMADs (Small Mother Against Decapentaplegic) and NFkappaB (Nuclear Factor kappa B) as well as the role of proliferation, differenciation and cell death in intestinal epithelial cells.
The gut is the largest and presumably most important immune organ of the body
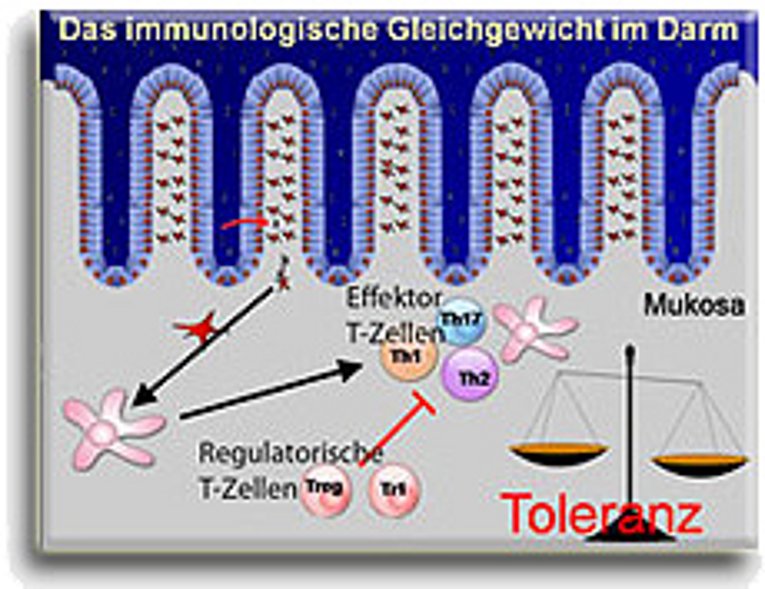
Underneath the epithelium, the gut harbors the cells of the intestinal immune system. It is estimated that about 80 % of all immune cells in the body are located in the gut. These cells act as watch-guards to recognize invading pathogenic bacteria and can mount strong immune responses to fight these intruders. During this battle, immune cells release various substances that drive inflammation and tissue destruction. To prevent an unwanted immune reaction against dietary components and harmless bacteria of the microflora, the basic setting of the intestinal immune system towards foreign antigens has to be tolerance. For maintaining immunologic tolerance in the gut, we currently believe that a special cell population named regulatory T cells is important. These cells control the activity of other immune cells in the gut and prevent inflammation. Our research group studies the molecular mechanisms by which these cells are generated and maintained in the gut. We have previously shown that such regulatory T cells can be induced in vitro by TGF-beta (Transforming Growth Factor-beta). Data of our group and other groups demonstrate that TGF-beta directly alters the genetic program of T lymphocytes in a way that they become regulatory T cells. We have also demonstrated that such in vitro induced regulatory T cells are capable of establishing immunological tolerance in the gut and can prevent intestinal inflammation. Reprogramming of human lymphocytes is an attractive concept for the treatment of patients with autoimmune and chronic inflammatory diseases. Our current research projects investigate molecules, responsible for the intracellular regulation of innate and adaptive lymphocytes in response to TGF-beta and other cytokines.
Selection of own studies:
1) Bao et al. Epithelial OPA1 links mitochondrial fusion to inflammatory bowel disease. Science Transl Med. 2025. 17(781):eadn8699.
2) González-Acera et al. Integrated multi-model analysis of intestinal inflammation exposes key molecular features of preclinical and clinical IBD. Gut. 2025 Apr 29:gutjnl-2024-333729.
3) Gámez-Belmonte et al. Epithelial Presenilin-1 drives colorectal tumour growth by controlling EGFR-COX2 signalling. Gut. 2023. 72(6):1155-1166.
4) Patankar et al. E-type prostanoid receptor 4 promotes resolution of colitis by blocking intestinal epithelial necroptosis. Nature Cell Biol. 2021. 23(7):796-807.
5) Günther et al. Interferon lambda Promotes Paneth Cell Death via STAT1 Signaling in Mice and is Increased in Inflamed Ileal Tissues of Patients with Crohn’s Disease. Gastroenterology. 2019. 157(5):1310-1322
6) He et al. Regression of apoptosis-resistant colorectal tumors by induction of necroptosis in mice. J Exp Med. 2017. 214(6):1655-1662.
7) Günther et al. Caspase-8 controls the gut response to microbial challenges by TNFalpha -dependent and –independent pathways. Gut. 2015. 64(4):601-610
8) Wittkopf et al. Cellular FLICE-Like Inhibitory Protein Secures Intestinal Epithelial Cell Survival and Immune Homeostasis by Regulating Caspase-8. Gastroenterology. 2013. 145(6):1369-79.
9) Günther et al. Caspase-8 regulates TNF-alpha-induced epithelial necroptosis and terminal ileitis. Nature. 2011. 477(7364):335-9.
10) Pickert et al. STAT3 links IL-22 signalling in intestinal epithelial cells to mucosal wound healing. J. Exp. Med. 2009. 206(7):1465-72.
11) Nenci et al. Epithelial NEMO/IKK-gamma links innate immunity to chronic intestinal inflammation. Nature. 2007. 29;446(7135):557-61.
12) Becker et al. TGF-beta suppresses tumor progression in colon cancer by inhibition of IL-6 trans-signaling. Immunity. 2004. 21(4): 491-501.